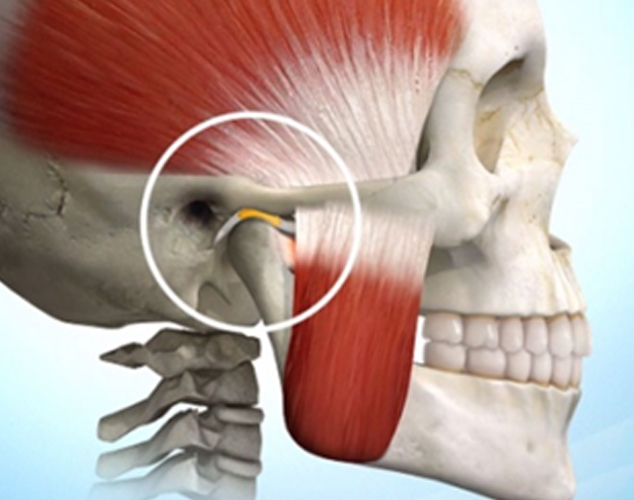
The most persistently used joint in the body, the temporomandibular joint (TMJ), is responsible for the movement of the lower jaw (mandible). Without this joint, which connects the lower jaw with the skull, we would not be able to open our mouths to eat, chew, breathe, or talk.
What is TMD?
TMD (Temporomandibular Joint Disorder) is characterized by pain and aching in the jaw, persistent clicking, limited range of motion and sometimes headaches or earaches. TMJ disorders may be mild to severe, short or long term.
Causes of TMJ Disorders:
Bruxism (grinding):
Often, people grind or clench their teeth at night while they are sleeping. This involuntary activity puts an enormous amount of pressure on the joint, creating inflammation.
Displacement or dislocation of the disk:
There is a disk in between the jawbone and the socket that can become displaced, dislocated or damaged, causing damage and pain.
Trauma:
An injury to any part of the jaw can cause pain in the joint.
Stress:
Painful spasms and trouble moving the jaw are sometimes the result of stress.
Minimally Invasive TMJ Treatment
- Treatment that avoids surgery or other invasive procedures and focuses on non-surgical management of symptoms.
- Night Guards and Splints
- Physical Therapy
- Home Care
- Soft Foods
- Anti-inflammatory medications
- Stress Management
- Relaxation Technique
Surgical Treatment
Surgery is often required for TMJ disorders that have not responded to non-surgical treatments.
Avoiding “open” joint surgery unless absolutely indicated
Incisions and surgery within the TMJ have risks and can lead to scarring that is best avoided if possible.
Arthrocentesis and Arthroscopy
Surgical procedures avoiding incisions and utilizing only 1-3 needle punctures around your TMJ to irrigate the site, remove harmful inflammation, and improve scarring that may be present.
Modified Condylotomy
A larger surgical procedure that allows the part of the jaw that is within the TMJ to “relocate” to the correct position without opening the TMJ or making facial incisions.
This procedure is performed in a hospital setting and requires at least 1 week off from work/school.
Open TMJ Surgery
Used as a last resort, Open TMJ surgery provides the benefit of direct visualization of the TMJ but is preferred as a last resort .
Frequently Asked Questions — TMJ Disorders & TMJ Arthroscopy
1. What is the temporomandibular joint (TMJ)?
The TMJ is the jaw joint that connects your lower jaw (mandible) to the skull. It allows chewing, speaking, swallowing, and facial movement.
2. What are the common symptoms of TMJ disorders?
Patients may experience:
-
Jaw pain
-
Clicking or popping sounds
-
Limited jaw opening
-
Muscle stiffness
-
Headaches
-
Ear pain or pressure
-
Locking of the jaw
-
Facial pain
3. What causes TMJ disorders?
Common causes include:
-
Trauma or injury
-
Teeth grinding (bruxism)
-
Jaw misalignment
-
Arthritis
-
Stress-related muscle tension
-
Disc displacement inside the joint
Sometimes, multiple factors contribute.
4. How are TMJ disorders diagnosed?
Diagnosis involves:
-
Detailed clinical examination
-
Jaw range-of-motion assessment
-
Palpation of joint & muscles
-
CBCT / MRI imaging
-
Bite and occlusion analysis
5. What is the first line of treatment for TMJ disorders?
Most TMJ problems respond to non-surgical management such as:
-
Bite splints / night guards
-
Physiotherapy
-
Anti-inflammatory medication
-
Muscle relaxants
-
Stress management
-
Soft diet & jaw rest
6. What is TMJ arthroscopy?
TMJ arthroscopy is a minimally invasive surgical procedure using a small telescope-like camera inserted into the joint.
It allows:
-
Direct visualization
-
Flushing of inflammatory fluid
-
Removal of adhesions
-
Repositioning of the disc
-
Treating joint inflammation
It is safer and less invasive than open joint surgery.
7. When is TMJ arthroscopy recommended?
Arthroscopy is recommended when:
-
Pain does not improve with conservative therapy
-
Jaw locking occurs
-
The disc is displaced
-
There is joint inflammation
-
The patient has restricted mouth opening
-
Imaging shows internal derangement
8. What are the benefits of TMJ arthroscopy?
Benefits include:
-
Small incisions (2–3 mm)
-
Faster recovery
-
Less swelling
-
Immediate improvement in mouth opening
-
Relief of joint pain
-
Minimal scarring
9. How long is the recovery after TMJ arthroscopy?
Most patients experience:
-
Mild swelling for 1–3 days
-
Return to normal activity within a week
-
Improved function within weeks or even days
10. Are there risks with TMJ arthroscopy?
Risks are low and may include:
-
Temporary numbness
-
Mild bleeding
-
Swelling
-
Rare infection
Compared to open joint surgery, risks are significantly lower.
11. Can TMJ arthroscopy cure clicking sounds?
If clicking is caused by disc displacement or adhesions, arthroscopy often reduces or eliminates it.
However, some residual clicking may remain but without pain.
12. Will TMJ arthroscopy improve mouth opening?
Yes — restoration of normal jaw movement is one of the major benefits.
13. When should I consider TMJ joint replacement?
Only for severe, end-stage joint damage (advanced arthritis, ankylosis).
Most patients improve with arthroscopy or conservative care.
Postoperative Instructions (TMJ Arthroscopy)
TMJ Arthroscopy — Postoperative Instructions
These instructions support a smooth and safe recovery after TMJ arthroscopy.
1. Pain & Swelling
-
Mild swelling for 1–3 days is normal
-
Use ice packs (20 minutes on, 20 minutes off) for the first 48 hours
-
Take prescribed pain medication on schedule
2. Diet
-
Start with soft diet (soups, yogurt, mashed food)
-
Avoid hard chewing for 1–2 weeks
-
Maintain adequate hydration
3. Jaw Exercises
-
Begin gentle jaw range-of-motion exercises as instructed
-
Do exercises 3–5 times daily
-
Gradually increase mouth opening over 2–3 weeks
4. Wound Care
-
Incisions are tiny (2–3 mm) and usually require minimal care
-
Keep the area clean and dry
-
Avoid touching incision sites unnecessarily
5. Activity
-
Avoid strenuous activity for 1 week
-
Sleep with head elevated for 3–5 days
-
Avoid extreme jaw movements (wide yawning, chewing gum)
6. Medications
Take all prescribed:
-
Antibiotics
-
Anti-inflammatory medications
-
Pain relievers
7. When to Call Your Surgeon
Contact immediately if you experience:
-
Increasing pain after 3 days
-
Persistent fever
-
Difficulty swallowing
-
Sudden jaw locking
-
Excessive bleeding
TMJ Disorders & TMJ Arthroscopy in Abu Dhabi, UAE — Advanced Minimally Invasive TMJ Treatment
TMJ disorders (TMD) affect millions worldwide and can cause jaw pain, clicking, headaches, ear fullness, and restricted mouth opening.
If you are searching for TMJ specialist in Abu Dhabi, TMJ arthroscopy UAE, or best TMJ surgeon, this page provides everything you need.
What Causes TMJ Disorders?
Common causes include:
-
Jaw joint disc displacement
-
Teeth grinding (bruxism)
-
Jaw misalignment
-
Arthritis in the joint
-
Trauma or overuse
-
Muscle tension
What Is TMJ Arthroscopy?
TMJ arthroscopy is a minimally invasive surgery where a small camera is inserted inside the joint to diagnose and treat internal problems.
It allows:
-
Disc repositioning
-
Removal of adhesions
-
Joint flushing (lavage)
-
Reduction of inflammation
Why Consider TMJ Arthroscopy?
-
Faster recovery
-
Small incisions (2–3 mm)
-
Immediate improvement in jaw function
-
Less postoperative pain
-
Excellent long-term relief
Treatments Offered
✔ Non-surgical treatments
✔ Splints & bite guards
✔ Botox for TMJ pain
✔ TMJ arthroscopy
✔ Open joint surgery (rarely needed)
Why Choose Dr. Thomas George Arayathinal?
Dr. Thomas is an internationally trained Consultant Oral & Maxillofacial Surgeon, with fellowship training in TMJ arthroscopy (Maryland, USA) and 30+ years of experience treating complex TMJ disorders.
If you suffer from jaw pain, clicking, headaches, or restricted opening, schedule a consultation today.